
Breast Cancer Awareness
Breast cancer is the most common cause of cancer in women, with one in 8 women developing breast cancer in their lifetime. Of these women, 75% do not have a family history or known risk factors. Breast cancer is also the number one cause of cancer-related death in women. However, if detected early, breast cancer is treatable. This is why breast screening is so important in the fight against this all too common disease.
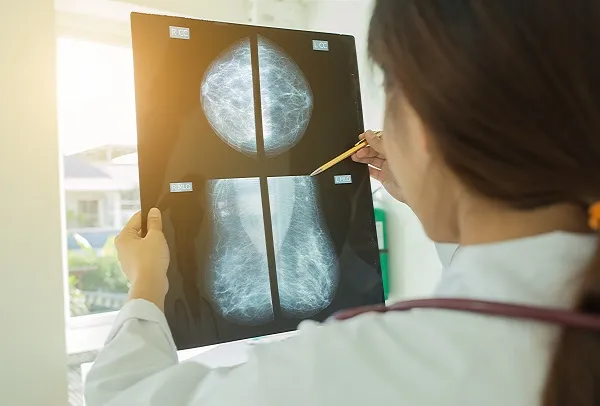
Early detection of breast cancer requires breast self awareness, including self examination, and screening with mammography and possibly ultrasound. It also requires knowing your personal lifetime risk of developing breast cancer, and assessing your family history, which guidelines to a breast MRI and/or genetic testing being recommended. Last, knowing the density of your breasts, which is the ratio of breast tissue compared to fat in your breasts, means you may need an ultrasound in addition to your mammogram.
According to the American College of Radiology, breast screening is recommended annually starting at age 40, or 10 years prior to a first degree relative diagnosed with the condition, whichever is earlier. If you are at high risk of developing cancer, screening is recommended earlier, usually starting at 35 in the UAE. If you are a BRCA gene mutation carrier, which is a known risk factor for developing breast and/or ovarian cancer, or your status is unknown and you have a 1st degree relative with BRCA gene mutation, then screening with MRI is recommended starting at age 25, and mammography starting at age 30. Screening imaging modalities include mammogram, which is the basis of screening, and possible supplementary ultrasound and/or MRI.

Risk assessment is usually based on a series of questions including previous biopsies, age at first birth, and family history. Family history is important, as certain forms of breast cancer can be hereditary. The most commonly used risk assessment tools are the GAIL model and IBIS models, with the IBIS model also incorporating your breast density. The model provides a percentage lifetime risk of developing breast cancer, with < 15% being considered average risk, 15 – 20% intermediate risk, and > 20% high risk. Based on your risk assessment, your radiologist and doctor can recommend the best screening program that is right for you.
In addition to imaging, it is important to know your breasts, and perform self examinations. The best place to examine yourself is in the shower, after your period has ended if premenopausal, or once a month. You can use the flats of three fingers to examine each quadrant of the breast with respect to the nipple. Don’t forget to check all the way to your breast bone, and all the way to the side, as many of us have breast tissue in these locations also. Also check up into the underarms for any enlarged lymph glands. Things to look for are lumps or masses, skin changes especially redness and swelling of the breasts and skin dimpling, nipple changes, and underarm swelling.
A diagnosis of breast cancer usually begins with your breast radiologist, who will perform a minimally invasive image-guided biopsy. There are many treatment options for breast cancer. The mainstay of treatment is surgery, and possibly chemotherapy, hormonal therapy and radiation therapy. Surgical options include a lumpectomy, if the cancer is localized to a small area, or mastectomy, which is removal of the whole breast. You will be treated usually by a team of breast specialists including the radiologist, surgeon, oncologist, and radiation oncologist.
Although we do not know the exact cause of breast cancer, many risk factors are known. It is important not to blame yourself if you are diagnosed with breast cancer. However, there are lifestyle factors that may help lessen your risk, including maintaining a healthy weight, adding exercise into your routine, limiting alcohol intake, limiting menopausal hormone use, and breast feeding if you can.
Talk to your doctor about your breast cancer risk, and incorporate breast self awareness, screening, and a healthy lifestyle into your routine, so we can achieve a world without breast cancer.










